Does IVF help us have more children?
How helpful is the reigning medical option for delayed parenthood?

When it comes to topics of fertility and infertility, we can’t really skip over IVF. It will inevitably come up quite a lot, actually, because it’s the reigning medical approach to any instance of delayed pregnancy plans (whether voluntary or involuntary).
Because of this, it’s also been discussed repeatedly in the political world over the last year as both Trump and Harris push for more readily accessible (and affordable) IVF for all. The Christian world hasn’t been silent either. Earlier this year, one of the world’s largest Christian denominations — the Southern Baptists — offered a resolution expressing concerns and encouraging members to seek IVF alternatives.
I’ve said it before and I’ll continue to say it — IVF is tough to talk about. IVF is personal. It’s sensitive. We think of couples who have long desired a baby, but due to unexplained infertility or recurrent pregnancy loss, have not been able to have them. We think of friends or family who are told by their doctors that their only hope for biological children is IVF.
For these beloved, we want to do all we can to help make this tender dream a reality!
But, does IVF actually do that?
How effective is IVF overall?
A recent article from the Institute of Family Studies provided some helpful data to understand the larger picture of the role IVF actually plays in forming our families:
In 2022, just 0.5% of births to women ages 25-29 involved IVF.
…most IVF users do not have high odds of going on to have more children: whereas 2.3% of first births in 2022 involved IVF, just 1.8% of second births and 0.9% of third births did.
…younger people…might possibly change their fertility behavior in expectation of using IVF in the future.1
There are other statistics out there, too, like the CDC’s National IVF Summary that show of the 413,776 IVF retrievals in 2021, only 97,128 pregnancies resulted. Even excluding the 36,072 egg retrievals that were for women desiring to freeze her eggs for future use, that still leaves the success of IVF at a disappointing 25% overall.
(I can’t help but also point out that this number only shows egg retrievals to successful live birth, not embryo transfers to successful live birth. For those paying for and living through each transfer, they recognize the difference.)
Maybe this is part of the reason why those in the 25% are so unlikely to go on to have another pregnancy through IVF?
What impact does age have on IVF?
Age also makes an incredible impact on the success of IVF. This should not be shocking, since female reproductive health changes — diminishes — with age. Yet, many women are promised results regardless of their age. They are encouraged to freeze their eggs in their 20s with the assumption that they’ll be able to easily utilize them in their 30s or 40s. They get the impression that their body and its functions are somewhat irrelevant to the process. This is not the case.
Egg quantity and quality have a direct impact on successful pregnancy, as does the ability of the uterus to create a healthy, supportive environment for pregnancy, and the ability of the corpus luteum to create sufficient levels of reproductive hormones. Medications and hormonal supplements play a role, but they cannot replace the function of the human body.
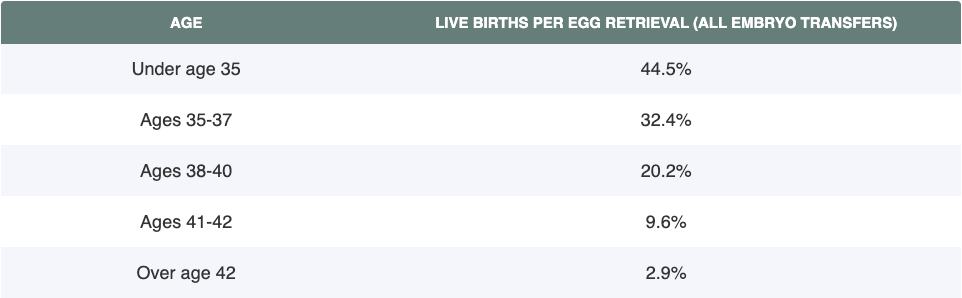
Look at this graph created by Forbes Health:
Look at how dramatically the numbers begin to reduce in 2 year increments. And yet, all ages “under 35” are lumped together. I can assure you, the success rate for a 24 year old will be different than that of a 34 year old, and yet the studies include them all together. This is misleading to women and couples seeking the next step in finding a solution.
(Once again, this study looked at live births per egg retrieval, not embryo transfer.)
Is IVF-for-All really the best answer?
For anyone who has walked through infertility or loved someone who has, we know that statistics aren’t really the decision-maker. When we’re heartbroken and desperate, we’re not looking for numbers, we’re looking for hope.
But the statistics are enlightening.
1 in 4 women will have a live birth after an unknown number of the embryo transfers involved after one egg retrieval. For some, this is encouraging, and for others, it’s disheartening.
Statistics make it very clear that IVF is not as successful for older couples, and yet it’s older couples who are most often told it’s their only option.
IVF is far more successful for younger couples (who may have issues that simply went undiagnosed or unaddressed and therefore more easily overcome).
But, statistics show us that broader access to IVF may influence younger couples to delay childbearing — which would then statistically make it more difficult for them to successfully have biological children.
We could take this conversation further, and talk about how this unlikelihood of success leads couples to use donor eggs, donor sperm, or surrogacy, but instead I think I’ll ask another question:
Is there more hope to be found elsewhere?
Not every couple will be blessed with biological children. Yet, every couple deserves the opportunity to prayerfully pursue it and receive dignified, compassionate care in the process.
The reality is that IVF is only one approach to infertility or recurrent pregnancy loss. IVF is easy to study (just look at the available statistics!) because each tiny aspect of the process can be isolated and tinkered with. Research abounds. But it’s not always the most dignified care for women.
I have the opportunity to speak with women who have walked this road and been left “like an empty shell that’s been used and experimented on without anything to show for it.”2
This cannot be the only option we give our struggling couples. And, thankfully, it’s not.
Instead of being a passive participant in the IVF process, women deserve to have a seat at the table — being an active voice in their reproductive healthcare.
Women deserve comprehensive care for reproductive health issues and infertility. They deserve to have infertility treated as a symptom, not a final diagnosis: What does it point us to? What’s going on behind the scenes?
Addressing these issues — through restorative care — actually optimizes the reproductive system, instead of trying to bypass or manipulate it. Not only does this improve the results, but it improves the woman’s quality of life. Shouldn’t our hope be that by the end of the process, women feel more knowledgeable, more empowered, and more improved than they did before?
Women are willing to do whatever it takes to become mothers, but what it shouldn’t take is their dignity.
But what about the statistics?
I’ll go ahead and acknowledge that there may not be as many studies on the effectiveness of restorative reproductive care, but they are most certainly out there. Let’s look at a just a few:
This study completed on women from two restorative reproductive medicine (RRM) clinics from 2004 - 2010 with a mean age of 35.7 who had a history of failed IVF showed a 32.1% success rate overall. For women 35-38, the live birth rate was 37.5% and women over 40 had a live birth rate of 27.4%. This study also showed that babies born through the RRM approach were less likely to have a premature birth, low birth weight, or be a part of a multiple.
There are numerous case studies, like this one, where a couple who had been trying to conceive for 16 years and had gone through 8 unsuccessful embryo transfers and experienced 3 recurrent pregnancy losses was able to successfully have a baby after only FIVE cycles with RRM patient-specific treatment.
When it comes to getting pregnant, the Restorative Reproductive Medicine approach is about getting pregnant “as healthily as you can, not as fast as you can.”3
Why should we settle for less?
Why do we promote methods that are not truly all that effective, when there are better options available? Why are we encouraging women to delay pregnancy, when their likelihood of success — even with IVF — reduces dramatically with each decade?
Sometimes it feels like a rushing river of popular opinion — one that’s impossible to navigate in any other direction. But our goal here is not to transform public opinion or be responsible for political law making (thank you, Lord). It’s to have honest, authentic conversations about issues that matter to women and couples. It’s to share with those across the table from us about options that they may not know about otherwise. It’s to invite God into the conversation — or remember that he’s been there all along.
Had you heard of Restorative reproductive medicine (RRM) before? What are your thoughts on RRM vs IVF? Did you know that the overall effectiveness of IVF was so low? Have you had personal experiences with either RRM or IVF? Does this information impact your views on infertility and its treatment? As always, I look forward to your thoughtful and charitable engagement in the comments!
Recent Podcast Episode:
As a reader, you likely value the work we’re doing at Fertile Faith: Thank you! Reading itself is a great way to support this work.
Here are a few other ways that can help keep us going:
Share this post! Do you have a friend who may benefit from these words? Share it with them!
Recommend Fertile Faith on Substack! If you have your own substack, then you know how Recommendations help us all. If you appreciate this work, consider recommending!
Subscribe and show us that you value the continued work and message of Fertile Faith by becoming a paid subscriber!
As a reminder, Fertile Faith is written by Caitlin Estes. Caitlin is the Owner and Certified FertilityCare Practitioner at Woven Natural Fertility Care, and feels passionate about providing empowering fertility education to women. Woven talks openly about the deep relationship between fertility and faith. As a Christian, Caitlin feels passionate about God’s good design of our bodies and fertility, and how this area of our lives can be incredibly fruitful, spiritually.
https://ifstudies.org/blog/mandating-insurance-coverage-for-ivf-will-not-boost-fertility?utm_source=substack&utm_medium=email
I recently had a conversation with a new client who is still recovering from the impact IVF had on her. Multiple retrievals, over 3 dozen embryos created, years devoted to the process, and no living children as a result. Come, Lord Jesus.
Quote from Dr. Phil Boyle, President of the International Institute of Restorative Reproductive Medicine, quoted here: https://www.realclearscience.com/articles/2024/04/26/restorative_reproductive_medicine_is_a_better_way_to_tackle_infertility_1027608.html







This was helpful info. Thank you 💖
Doing the Lord's work here!